Hospital opens second COVID-19 unit
- Category: Health & Wellness, Community
- Posted On:
- Written By: Deb Sutton, Sweetwater Memorial Public Information Officer

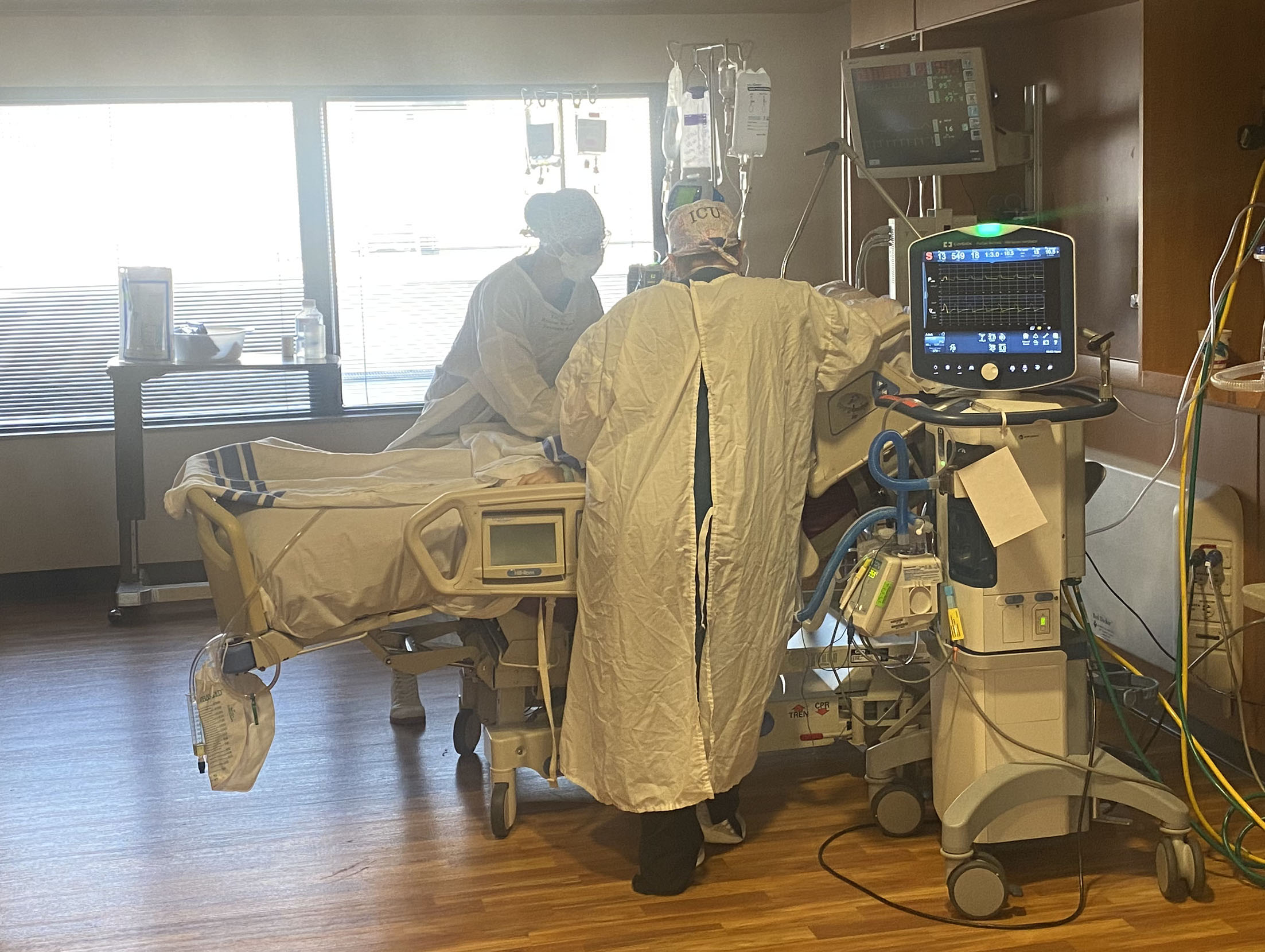 Through the protective class of an ICU suite, ICU nurses Kimber Burger, left, and Krindell Shepard check on a patient Tuesday afternoon at in the ICU Unit at Sweetwater Memorial.
Through the protective class of an ICU suite, ICU nurses Kimber Burger, left, and Krindell Shepard check on a patient Tuesday afternoon at in the ICU Unit at Sweetwater Memorial.
Surge in seriously ill patients hits during Labor Day weekend
During the Labor Day holiday weekend, Memorial Hospital of Sweetwater County’s Incident Command initiated another step in its COVID-19 Surge Capacity Plan.
This tiered plan has been in place since the Incident Command System for the pandemic first formed in early March 2020.
The hospital’s ICU had already been designated a COVID unit. With the increase in seriously ill COVID-19 patients, it was necessary to designate the same-day surgery department as a second COVID unit, said Deb Sutton, MHSC Public Information Officer.
With same-day surgery now being used as a COVID unit, elective surgeries will continue to be put on hold, Sutton said.
COVID-19 activity increased in the emergency room Friday. A number of COVID patients were admitted throughout the weekend, peaking with 19 COVID inpatients by Sunday morning. COVID-19 accounted for 73% of all patients in the hospital. Of those, about 90% were unvaccinated, Sutton said.
Throughout the weekend, physicians, nurses and other members of the MHSC healthcare team stepped in to help move beds and make room for the additional COVID patients in same-day surgery, Sutton said. Many people from other departments, along with several who came in on their days off, pitched in to help. During this, staff continued to care for the six to seven non-COVID patients housed on the medical/surgical floor.
“Staffing is one of the hospital’s biggest issues right now,” said MHSC Chief Nursing Officer Ann Clevenger. “This last week was tough.”
As of Tuesday morning, the hospital had 16 COVID-19 patients. Of those, about 87% are unvaccinated.
Here are some averages (fiscal years run from July to June) including all inpatients from different time periods to help lend some perspective:
Average Daily Census
- FY 2018-19 prior to the pandemic: 12.6
- FY 2019-20 including start of the pandemic: 11.0
- FY 2020-21 during pandemic: 11.4
- November, December, January 2021: 13.8
- Last three months: 11.2
- Last two weeks: 17.4
Average Length of Stay
- FY 2018-19 prior to pandemic: 2.9
- FY 2019-20 including start of the pandemic: 2.8
- FY 2020-21 during pandemic: 3.0
- November, December, January 2021: 3.6
- Last three months: 3.1
- Last two weeks: 4.9
“Recently, with the delta variant surge, our hospitalized patients with COVID-19 are requiring longer stays and more intensive care than we see with many other illnesses,” said MHSC Chief Medical Officer Dr. Melinda Poyer. “With these variants, people are getting significantly sicker in a shorter amount of time. It is hard to predict which patients will feel symptoms no worse than a cold, and which ones will progress and end up in intensive care, particularly now that it is affecting the younger age groups so heavily. In the last two weeks, we have, unfortunately, had to admit patients in their 30s, 40s and 50s for intensive care.”
The age of COVID-19 patients now being seen in the Emergency Room has ranged from infants to the elderly, said MHSC Incident Commander Kim White, Emergency Services Director.
“With this variant, we are treating many patients in their 30s to 50s,” White said. “We have diagnosed infants with COVID-19. We had one we thought for sure would come back as an RSV diagnosis, since we are seeing RSV (respiratory syncytial virus) much earlier this year.”
“Everyone is at risk,” said Dr. Phil Najm, MHSC Emergency Medical Director with University of Utah Health. “We are sending patients home on oxygen each day who in different times would be able to be admitted. Some of them can recuperate at home, but some of them worsen and return in just a few days needing life support; some die despite receiving advanced life support.
“People should understand that the hospitals where we would typically transfer the most critical patients are full,” Najm said. “The surge likely will get worse over the next two to four weeks. It would not be like this if more people were vaccinated.”
White said the crisis is taking a toll on MHSC staff.
“Everyone can see the toll the pandemic and the workload is taking on each of our staff members,” she said. “We see the weary look in their eyes, and the slowing of their steps. We understand the feelings of defeat, and the feeling that few outside of our walls are paying attention to what is going on.”
For more information, go to the Coronavirus Update page at sweetwatermemorial.com.
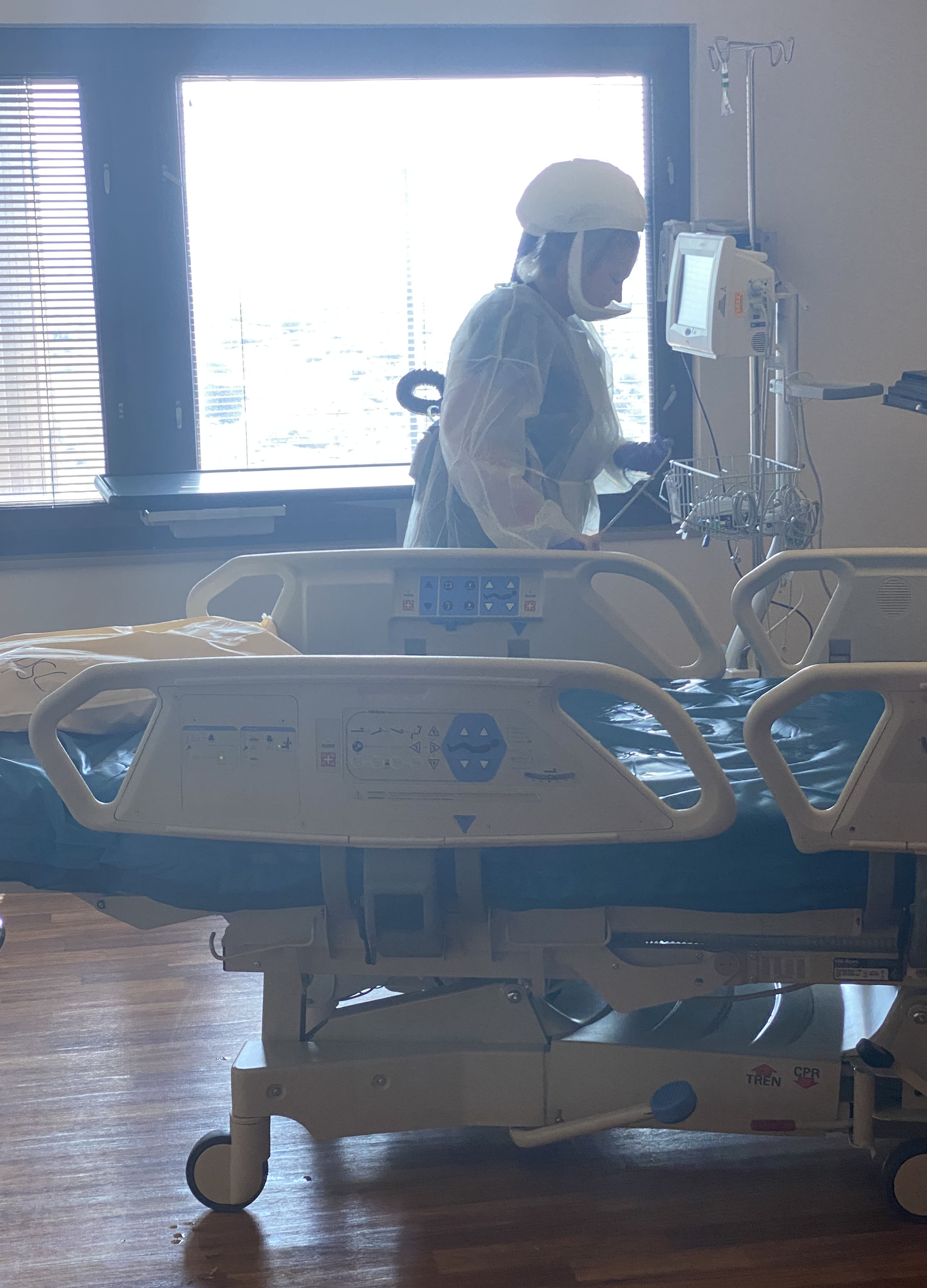
BELOW: Through the protective glass of the ICU rooms, MHSC Environmental Services worker Kristie Moore can be seen cleaning an ICU room Tuesday afternoon after a patient is discharged.